However, it takes no less than the whole day to get the results, and we are lacking resources to perform such test to detect viral RNA in each case. In the meanwhile, even mild COVID infections may develop into pneumonia within days and even hours. Pneumonia, in turn, often develops into respiratory failure and acute respiratory distress syndrome, which may be fatal for some patients.
Is it possible to detect COVID in X-ray images?
As the virus is unpredictable and very aggressive, scientists keep searching for new methods to detect this dangerous disease. While at the beginning of the current pandemic it was believed that X-ray cannot show coronavirus infection, today specialists have reconsidered this opinion.
Does X-ray identify coronavirus in the lungs? Some studies report that the tissues involved were visible in images in 9 of 10 cases. All radiography methods including X-ray are based on the ability of the beams to change their intensity as they are passing through tissues of different density. The beams reflect from light-sensitive film and transfer images of the organs to it.
Dark areas mean indurations and light areas represent cavities filled with air or fluid. In order to more accurately assess the status of the respiratory tract, specialists perform X-ray in two and more views.
Effectiveness of the Study
It’s no secret that X-ray exposure is harmful for the human body. However, the study lasts for no more than 1-2 seconds and, thus, the dose absorbed by the body is negligibly low. Therefore, the benefits clearly outweigh the risk. Adults can submit to X-ray studies up to several times a week if it is required for diagnosis and monitoring of efficiency of management of pneumonia.
The capability of X-ray study in terms of detection of involvement of the lungs with coronavirus infection was proved by Chinese researchers at the very beginning of the pandemic. X-ray is capable of detecting changes characteristic of the new infection. This is a simple, affordable and readily available method which can be used, if indicated, to evaluate almost any patient. At the present moment all polyclinics are equipped with X-ray machines, including portable systems which are easy to use at the patient’s bedside.
- However, abnormal changes will be detectable in X-ray images no earlier than 10 days after the patient contracted the infection.
It should be noted that CT or computed tomography is the most yielding imaging method which can detect coronavirus at early stages. CT is also a radiodiagnostic method but its images are in 3D format.
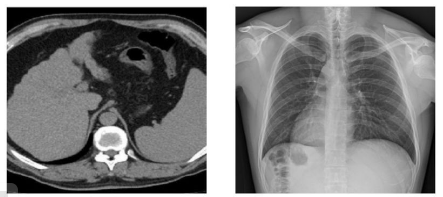
CT x-ray
However, CT is a more expensive and complex imaging technique. It may not be affordable for some patients, and there are just a few facilities in our country which can provide such services for free. Moreover, CT has some disadvantages, too – the radiation exposure in the process of such study is much higher.
How do the lungs look like in X-ray images?
Examination of images of now multiple COVID patients provided for determination of the most common features of involvement of the lungs in COVID:
- Disrupted lung alveolar structures on the background of inflammation – the lungs are involved bilaterally;
- Development of induration preconditioned by accumulation of inflammatory exudate, that is fluid mixed with mucus and blood. Such indurations are usually detected in both lungs across their surface;
- Fluid accumulates between the lungs and chest and forms so called “pleural effusion”;
- The pulmonary pattern is intensified;
- Lesions are mostly localized on the periphery, father from the heart and closer to the chest wall; and
- Ground glass opacities are detectable – the lungs become less dense and seem to be coated with opaque film.
The last symptom, ground glass opacities, is most commonly detectable with X-ray – almost a half of all studies help to identify it. However, CT is a better way to detect it. Nevertheless, X-ray is a rather reliable method to show this symptom.
Ground glass opacities look like large shadows since the lung surface becomes indistinct and seems to be blurry. This effect is related to obstruction of air flow into alveoli, which become poorly aerated with their walls thicken.
X-ray is a rather informative diagnostic method, but it is feasible only at the stage at which coronavirus reaches and involves the lungs. The PCR (polymerase chain reaction) method is still the only diagnostic tool which is effective at early stages.
Post-coronavirus lungs
After the disease some areas of the lungs may become indurated as the healthy tissue is replaced with fibrotic tissues. The function of the lungs becomes impaired and any physical stress which used to be a piece of cake before the disease may cause shortness of breath afterwards.
The inflammation process will relieve step-by-step, which normally takes some 2 weeks. After recovery, when no viral particles enter patient’s blood and when PCR tests are negative, their lung function will be impaired by about one-third.
Such impairment is attributable to the fact that the rigid fibrous tissue cannot open completely. These are the manifestations of pulmonary fibrosis, the danger and implications of which are yet to be investigated.
We still don’t know whether the lungs can recover from this, and if yes, whether such recovery can be complete. Right now, medical specialists cannot rule out irreversibility of this fibrous process and, thus, all COVID patients should be followed up by a pulmonologist for at least 6 months.
Risk factors associated with fibrous transformation
Some COVID patients do not have lung fibrosis. The factors increasing the risk of scar tissue growth include:
- Large lesions involving more than a half of a lung;
- Severe pneumonia accompanied by acute respiratory distress syndrome (ARDS);
- Mechanical ventilation of the lungs;
- Cases when the patient contracts secondary bacterial infection.
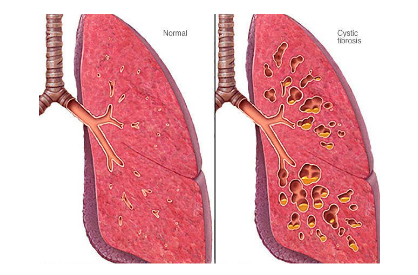
In fibrosis, the lungs become scarred, which impairs their ability to saturate blood with oxygen.
If COVID-19 was mild or moderate and if it was managed timely and properly, then fibrosis is unlikely to develop. This is a well-established fact as post-COVID patients are evaluated by performing X-ray, fluorography or computed tomography.
The former two studies are performed if there are no signs of respiratory failure, shortness of breath and severe heart palpations when the patient is moderately physically active. X-ray and fluorography are also recommended to patients for whom checkup evaluation does not reveal any residual manifestations in the lungs and whose blood tests show no inflammation.
Checkup imaging is performed 3 to 6 months after discharge from hospital. If a study reveals any induration, the patient should be followed up by the district pulmonologist. The doctor will prescribe a cycle of rehab therapy and advise the patient on submitting to CT or X-ray to monitor efficiency of such therapy.
Advantages of X-ray in coronavirus diagnosis
|
Study |
Accuracy, % |
Availability of results |
Availability of equipment |
|
X-ray |
>80 |
Max. within several hours |
All hospitals and polyclinics are equipped with X-ray machines |
|
PCR test |
More than 60 some studies may yield false positive and false negative results |
2 and more days |
We don’t have enough PCR test kits; you will need a referral card from your doctor |
Tips on when you should submit to X-ray
Tip No.1
There’s no sense in doing X-ray at early stages. It will do you no good both in the incubation period lasting for 2 to 14 days after you contracted the disease and when the first symptoms (fever, muscle aches and cough) appear.
X-ray is feasible when the symptoms become intense. In this case, it will be highly informative and beneficial.
Tip No.2
If you have had contact with someone having COVID and, thus, you may have contracted the infection, you need to visit your doctor. If any typical symptoms appear, you should better call your doctor to be evaluated at home.
- Attention! If you have body temperature above 38.5°C, long-standing cough attacks and shortness of breath, you should call an ambulance.
PCR tests are performed twice for the contacts and in case of suspected COVID. If there are typical signs, the test will be performed another two times even if the previous test was negative.
FAQ
Are there any novel methods being developed, which would provide for more prompt and accurate detection? At the present moment, even PCR test is far from being 100% accurate.
For many years companies such as Google and IBM, which are at the leading edge of technology, have been involved in development of a specific artificial intelligence (AI) capable of analyzing X-ray images. This will facilitate the diagnostic process and reduce the risk of human error.
- Alibaba, a technology giant, has already announced an AI system capable of detecting COVID-19 within 20 seconds.
In addition, the neural network will help specialists to eliminate the so called “search satisfaction”, when a specialist sees an issue in an image and diagnoses the patient without ruling out other possible diagnoses. As a result, the patient may be diagnosed with a wrong disease, which may be crucial for the patient since the issue detected may not be a symptom of the principal abnormality.
Latest trials conducted by researchers from Canada have shows high sensitivity and accuracy of COVID detection using AI. The authors have reported accuracy of 83% and, at the same time, the neural network in their studies was able to detect ground glass opacities and localize inflammation.
What is the difference between COVID-caused pneumonia and common pneumonia?
Bacterial pneumonia involves some parts of the lungs, while COVID-caused pneumonia affects the entire lungs. When SARS-CoV-2 reaches the lungs, the latter become poorly aerated and filled with inflammatory exudate (fluid).
Furthermore, common pneumonia can be treated with antibiotics, while we still don’t have any cure killing the COVID virus.


